Gestational Diabetes: Causes, Symptoms, And Treatment

Pregnant woman takes her blood glucose level with a glucometer to ensure maternal and fetal health.
Gestational diabetes is a form of diabetes that is specific to pregnancy and usually occurs during the second or third trimester. This condition is defined as an inability to produce sufficient insulin to overcome the increased requirements of pregnancy,y which results in increased blood glucose.
Gestational diabetes may not always show any symptoms; however, if left unchecked, it can pose dangers to the health of both mother and baby. With early diagnosis and adequate treatment, it is not a condition that will cause complications, and an understanding of the signs and symptoms, reasons why, and treatment of the condition is important to promote health in pregnancy.
What Is Gestational Diabetes?
Gestational diabetes mellitus (GDM) refers to the onset of hyperglycaemia initially detected during pregnancy, usually between 24 and 28 weeks. It develops when hormones from the placenta disrupt normal insulin activity. This leads to insulin resistance and impaired glucose uptake.
GDM is unique as it only develops from metabolic changes specific to the pregnancy State (unlike pre-existing diabetes mellitus), and many women present asymptomatically but have a risk of fetal macrosomia and pre-eclampsia if poorly controlled.
An oral glucose tolerance test should be used as a screening method. Early detection, management through lifestyle modification, exercise, and medical management results in effective glucose control and normal pregnancy outcomes in the majority of women.
Causes of Gestational Diabetes
Gestational diabetes happens because of the combination of hormones and metabolic changes that occur during pregnancy, which have an impact on insulin use in the body.
Hormones produced by the placenta in the mother's body,y which are used to help the baby grow, can make the mother more resistant to insulin.
Because the cells of the mother's body become resistant to insulin, they will not respond properly to it, which means the mother's blood glucose levels will rise. If the mother's pancreas can not produce enough insulin to compensate for this resistance, then gestational diabetes occurs.
The causes of gestational diabetes are often due to the combined effect of the following risk factors:
- Hormones produced by the placenta cause insulin resistance.
- Failure of the pancreas to produce enough insulin.
- An overweight or obese mother before pregnancy.
- Previous diabetes in the family.
- Mother has had gestational diabetes previously.
- An aged or older mother
Combined, these forces disrupt the body's normal glucose balance, causing blood sugar to increase during pregnancy.
Symptoms Of Gestational Diabetes
For many women with gestational diabetes, there are no noticeable symptoms, so it is often diagnosed through a standard screening test carried out during pregnancy. The signs that may be present in other women are generally mild and may be easily confused with normal symptoms of pregnancy.
Symptoms often include:
- Frequent need to urinate that does not appear related to pregnancy.
- Increased thirst and a dry mouth.
- Feeling persistently tired and listless.
- Nausea or a general feeling unwell.
- Blurred vision is, in some cases, reported as a symptom.
As many of the symptoms of gestational diabetes could be easily confused with normal pregnancy symptoms, a routine screening test is important for many women.

Pregnant woman sits on a bed with a pained expression holding her stomach showing her nausea symptoms from pregnancy with gestational diabetes.
Treatment For Gestational Diabetes
1. Monitoring and Medical Care
- Care in gestational diabetes is characterized by routine prenatal visits where the well-being of both mother and fetus is closely evaluated.
- Ultrasound studies are often done to monitor fetal growth, and frequent blood glucose levels are analyzed to detect potential complications such as Macrosomia.
2. Monitoring Blood Glucose Levels
- A woman with gestational diabetes is expected to check her blood sugar levels daily. Self-monitoring requires a glucose meter to obtain fasting and postprandial readings.
- Keeping blood sugar within prescribed limits (95 mg/dl fast; 140 mg/dl one hour postprandial; 120 mg/dl two hours postprandial) will minimize risks to mother and fetus.
- The readings taken should be recorded and submitted to the health care provider.
3. Lifestyle and Diet Modification
- Healthy diet and lifestyle changes are cornerstones in the treatment of gestational diabetes. Balanced and portion-controlled meal plans with protein, fiber, and healthy fats are necessary.
- Sugary drinks and processed food must be avoided, and small, frequent meals taken at the appropriate time will maintain stable blood sugar levels.
- Appropriate and consistent physical activity is a major element of the care in gestational diabetes and contributes significantly to increased insulin sensitivity.
4. Medication and Insulin Therapy
The management of gestational diabetes with drugs, particularly insulin therapy, is a necessary component when lifestyle changes are not adequate in achieving the required control.
When To Seek Medical Assistance?
- An abnormally increased thirst and frequency in urination beyond normal pregnancy symptoms.
- Unusual fatigue or weariness during routine daily activities.
- Blurred vision or uncontrollable nausea.
- A rapid weight gain or an unexplained large amount of weight gain during pregnancy.
- A family history of diabetes or a history of Gestational Diabetes in previous pregnancies.
- Difficulty in keeping the blood sugar levels within the acceptable limit.
- A decreased amount of fetal movements or excessive fetal movements.
- Any abnormality reported at the routine prenatal examinations.
The earlier the patients seek help, the faster the problem can be diagnosed.

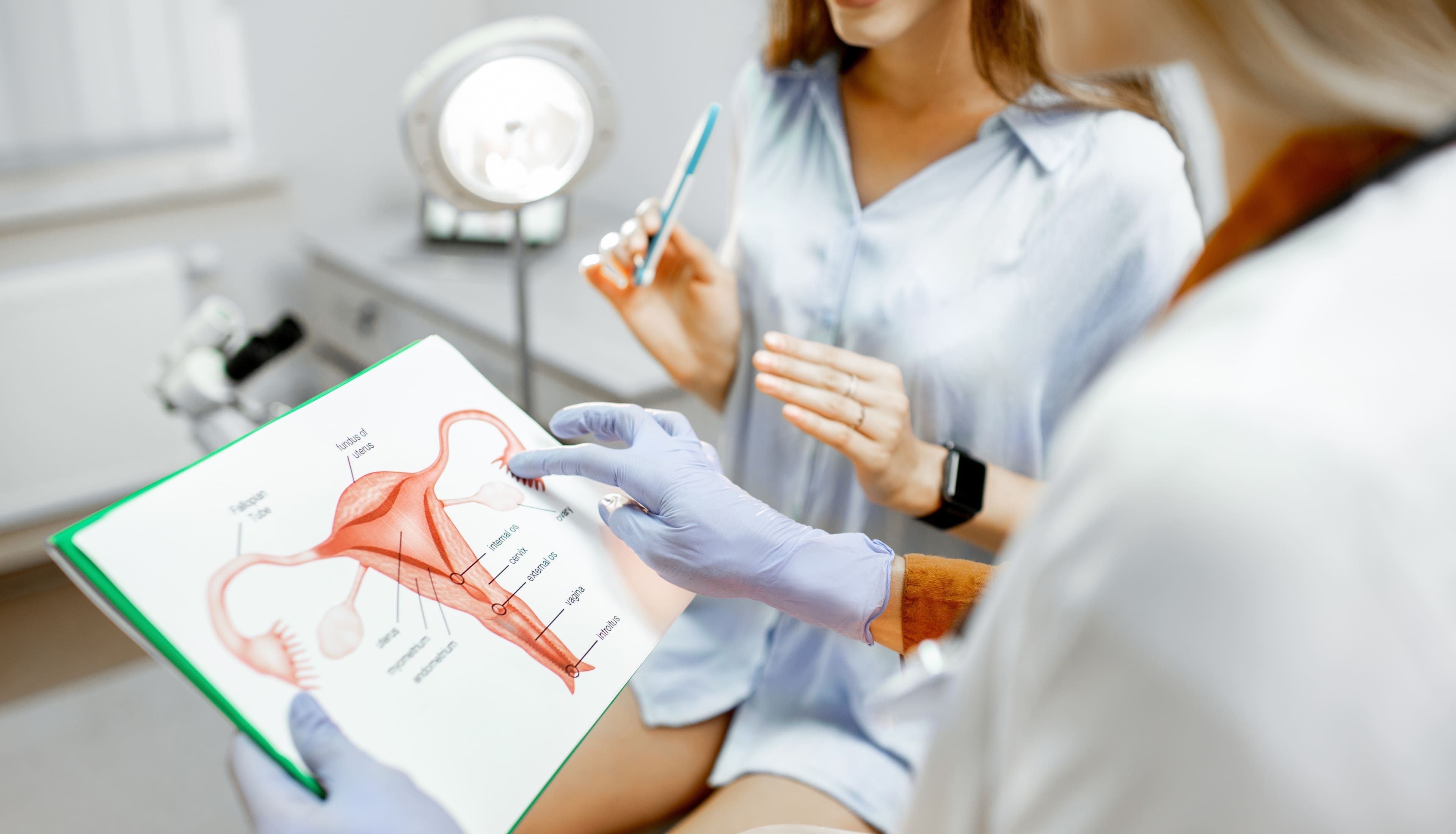
A doctor is shown explaining to a pregnant woman about gestational diabetes treatment and the necessary changes.
Final Thoughts
Gestational diabetes can be successfully managed with early detection and appropriate management strategies. Even though it arises because of hormonal changes related to pregnancy, the risks and complications of gestational diabetes can be controlled with monitoring blood sugar levels, a healthy diet, exercise, and medication when advised by the medical practitioner.
An early diagnosis and the prescribed management for gestational diabetes can significantly reduce the risk of complications to the mother and the child. Most women with gestational diabetes can still have an uncomplicated pregnancy and a safe delivery. Early screening, identification, and proper follow-up are extremely important for expectant mothers.
Expert Care With Dr. Shachi Singh
Dr. Shachi Singh is a senior consultant obstetrician and gynecologist based in Noida and an accomplished laparoscopic surgeon with over fifteen years of extensive experience in the field of women's healthcare. She provides complete care for gestational diabetes and offers accurate diagnosis and a customized diet and lifestyle advice, as well as blood sugar monitoring and medical management through effective procedures.
Patients trust her for safe pregnancy care, high-risk pregnancy care, and advanced laparoscopic procedures with the highest degree of accuracy and a humanistic approach. So, book your consultation today.
Frequently Asked Questions(FAQs)
1. Have I got a high-risk pregnancy with gestational diabetes?
Definitely, gestational diabetes is a high-risk pregnancy because it enhances risks for pre-eclampsia, macrosomia, and problems during delivery, so it needs a higher level of observation.
2. Is it still possible to have a healthy baby with gestational diabetes?
Yes. With control of blood glucose levels, a healthy diet, proper blood-sugar monitoring, appropriate medical care, and knowledge, most women with gestational diabetes give birth to healthy babies without any problems. Most women who can manage their condition effectively have healthy children with minimal health risks at birth and afterward.
3. When managing gestational diabetes, which foods should you avoid?
Foods to avoid include those that quickly raise your blood sugar. This includes things like sweet drinks, sweets, white bread, and white processed foods (like pasta), fried food, and any unhealthy snacks that have a high glycemic index. Fruit juices should also be limited, as should sweets.
4. How soon after delivery can I expect my gestational diabetes to clear?
Gestational diabetes will usually disappear after the birth, but blood sugars should be retested 6-12 weeks after delivery.