Endometriosis: Early Signs And Treatment Options

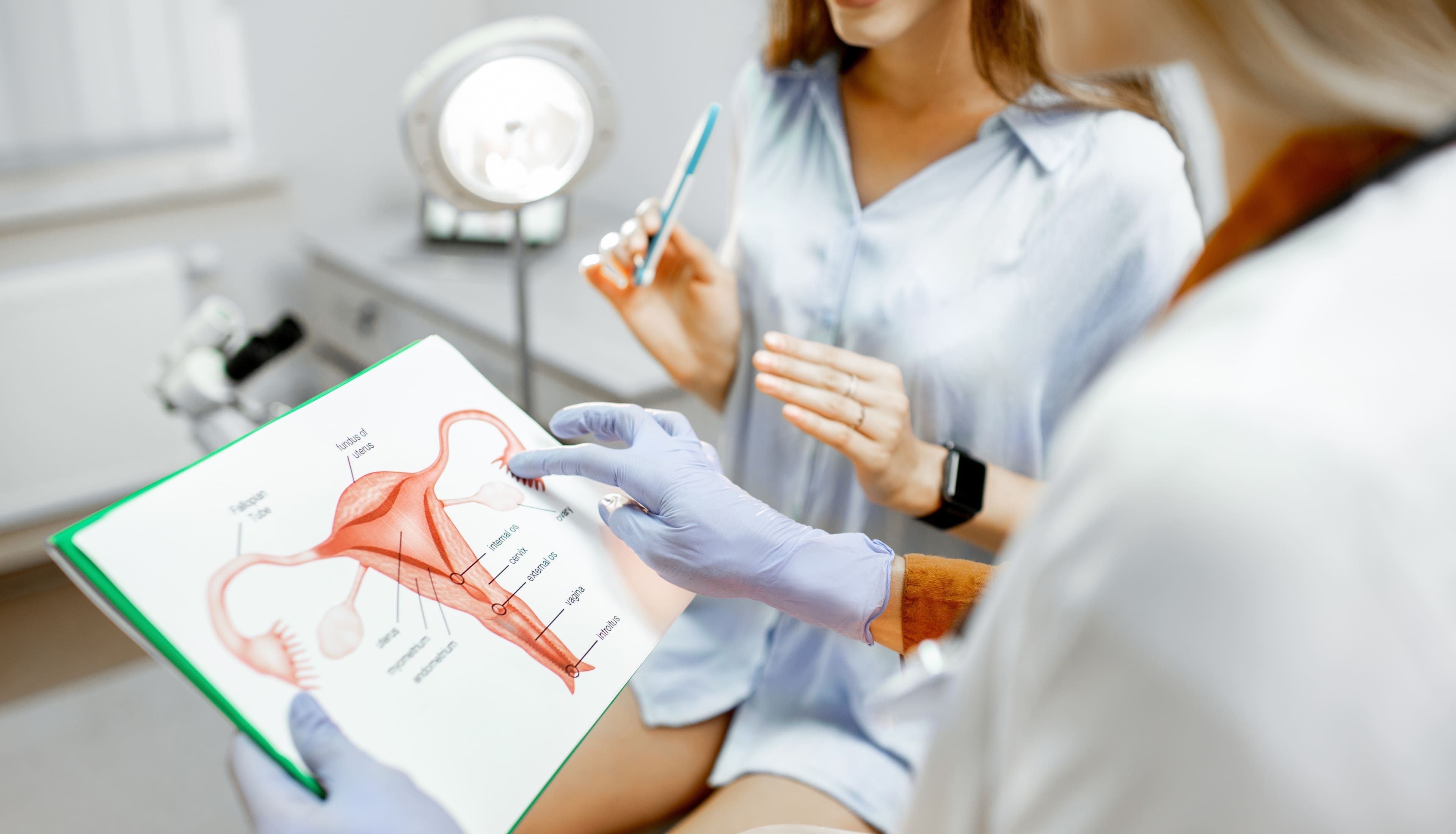
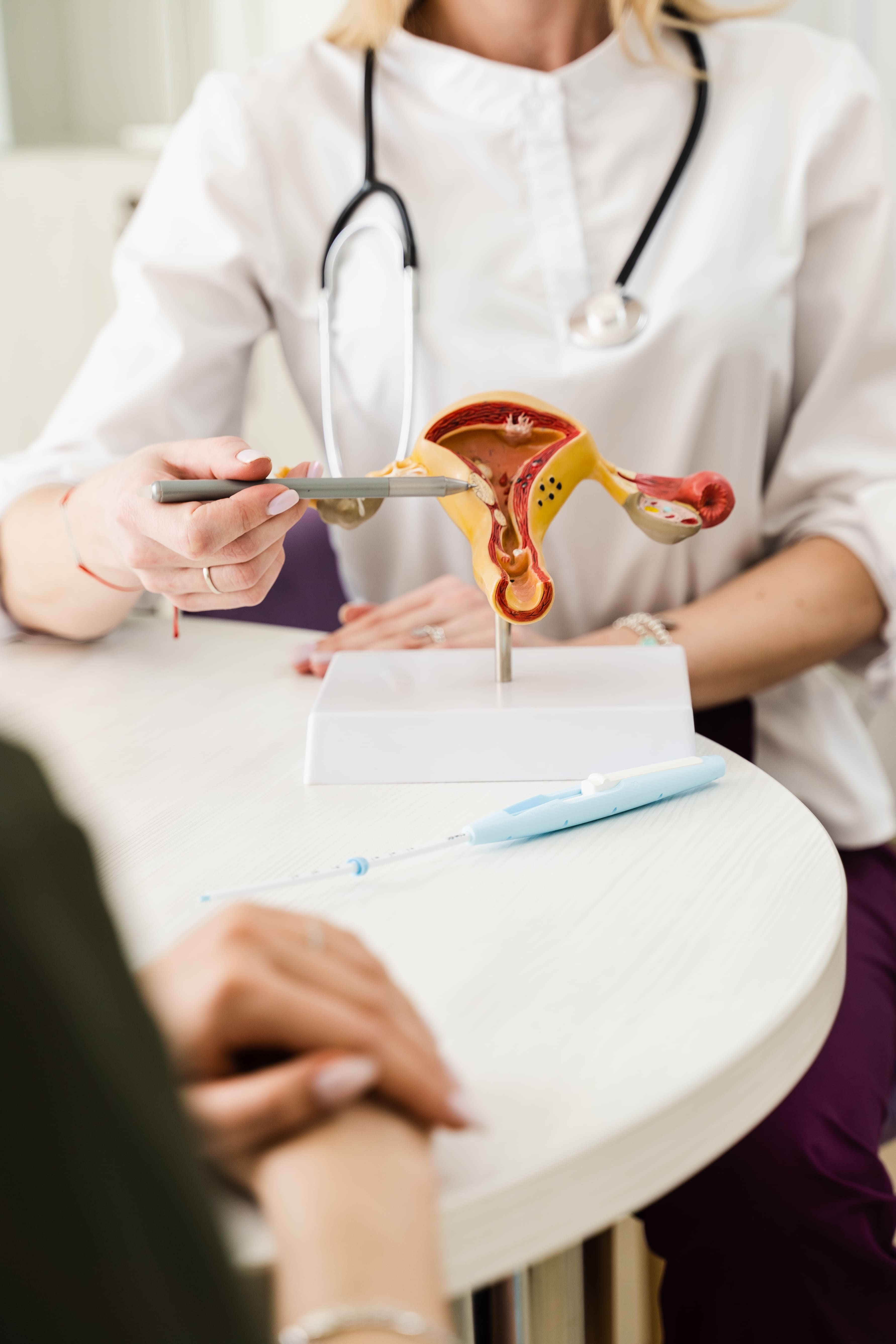
A woman sits down to discuss her symptoms with a gynecologist who carefully listens and gives her information about treatment and care of endometriosis.
Endometriosis, also known as a gynecological condition that affects women mostly during their childbearing years, is a disease in which tissue similar to endometrium is formed outside the uterus. It causes inflammation of the tissues involved, pain, and may even interfere with women's fertility. Due to a similar presentation in comparison to many other conditions, endometriosis often goes unrecognised and undiagnosed.
Knowing the initial signs, such as the occurrence of pelvic pain, dysmenorrhea, and vaginal bleeding, ng can result in a prompt diagnosis. The diagnosis as well as treatment of endometriosis can be approached medically as well as surgically, and advances made in treatments have enabled the better management of this disease as well as its effects on women's health and fertility.
What is Endometriosis?
Endometriosis is a chronic gynecological disorder in which tissue resembling the endometrial lining of the uterus grows outside its normal location. These abnormal growths commonly occur in areas such as the ovaries, fallopian tubes, peritoneum, the space behind the uterus, and occasionally within the uterine muscle (myometrium).
Less commonly, lesions may develop in distant sites, including the bladder, intestines, rectum, diaphragm, vagina, or lungs. This misplaced tissue responds to hormonal changes, leading to inflammation, pain, and scarring. Over time, it may interfere with reproductive function, potentially causing infertility due to adhesions and fallopian tube obstruction.
Symptoms of Endometriosis
A variety of signs and symptoms are associated with endometriosis, but the most common complaint is pelvic pain. This pain can range from mild to severe, and usually gets worse before and during menstruation because of the hormonal fluctuations and inflammation.
Many women complain of extremely painful periods as well as low abdominal or lower back pain, which can be present before, during, and between periods. Heavy or irregular periods, as well as spotting, are also common. Painful intercourse (dyspareunia) is another characteristic sign. Infertile women may present because of an inability to conceive.
Other, less specific symptoms may include painful urination or defecation and the presence of bowel symptoms such as bloating, diarrhea, and constipation. Some people with endometriosis do not develop any symptoms at all, and there appears to be no clear relationship between the amount of endometriosis present and the level of pain experienced.
The Main Symptoms Are:
- Very painful menstrual cramps
- Pelvic/abdominal/back pain
- Heavy or irregular bleeding
- Pain during intercourse
- Infertility
- Painful passing of urine/faeces
- Digestive symptoms (bloating, diarrhoea, constipation)

A mournful-looking couple sits beside each other, exhibiting concern and emotional discomfort about infertility caused by their endometriosis.
Causes of Endometriosis
1. Retrograde Menstruation
The flow of menstrual fluid back through the fallopian tubes into the pelvic cavity leads to implantation and proliferation of endometrial-like cells.
2. Coelomic Metaplasia
Peritoneal cells may transform into endometrial-like tissue following exposure to appropriate stimuli, thereby contributing to lesion development.
3. Immune System Malfunction
The body's immune system is likely defective, being unable to remove ectopic endometrial tissue.
4. Hereditary Factors
There is an increased risk in those with a positive family history.
5. Lymphatic or Hematogenous Spread of Endometrial Tissue
This theory proposes the spread of endometrial cells through the lymphatics or the bloodstream to remote sites.
6. Hormonal Factors
Estrogen promotes growth and maintenance of endometrial implants, aggravating disease progression.
7. Stem Cell Theory
Endometrial or bone marrow stem cells have been proposed to differentiate into ectopic endometrial tissue.
Treatment for Endometriosis
Management strategy aims at pain relief, reduction of progression and preservation of fertility as appropriate to patient preferences and reproductive potential.
1. Medications
- Analgesic drugs, such as Ibuprofen and Naproxen, are first-line treatments for relief of inflammation and pain caused by dysmenorrhea.
- These drugs should be taken at the onset of pain. In case of moderate and severe pain, analgesics may be combined with hormones for improved symptom management.
2. Hormonal therapy
- Hormonal therapies suppress ovulation and lower the level of estrogen in the body, which helps in controlling the growth and bleeding of endometrial tissues.
- Hormone treatments are divided into combined hormonal contraceptives, progestins, GnRH analogues, and aromatase inhibitors.
- Symptoms are controlled by hormonal therapy; it cannot cure the condition.
3. Surgical Management
- Laparoscopic (conservative) surgery: Involves removing endometrial tissue, but keeping the uterus and ovaries intact, which can help improve pain and fertility outcomes.
- Hysterectomy: Considered as a last resort, if there are severe symptoms of endometriosis, the uterus and possibly the ovaries are removed.
4. Fertility treatment
- The management of infertility will include the use of ovulatory-inducing drugs to promote egg formation.
- The reproductive technologies, such as the in vitro fertilisation technique, are the main treatment in severe cases of infertility with the condition, and if treatment is not successful.

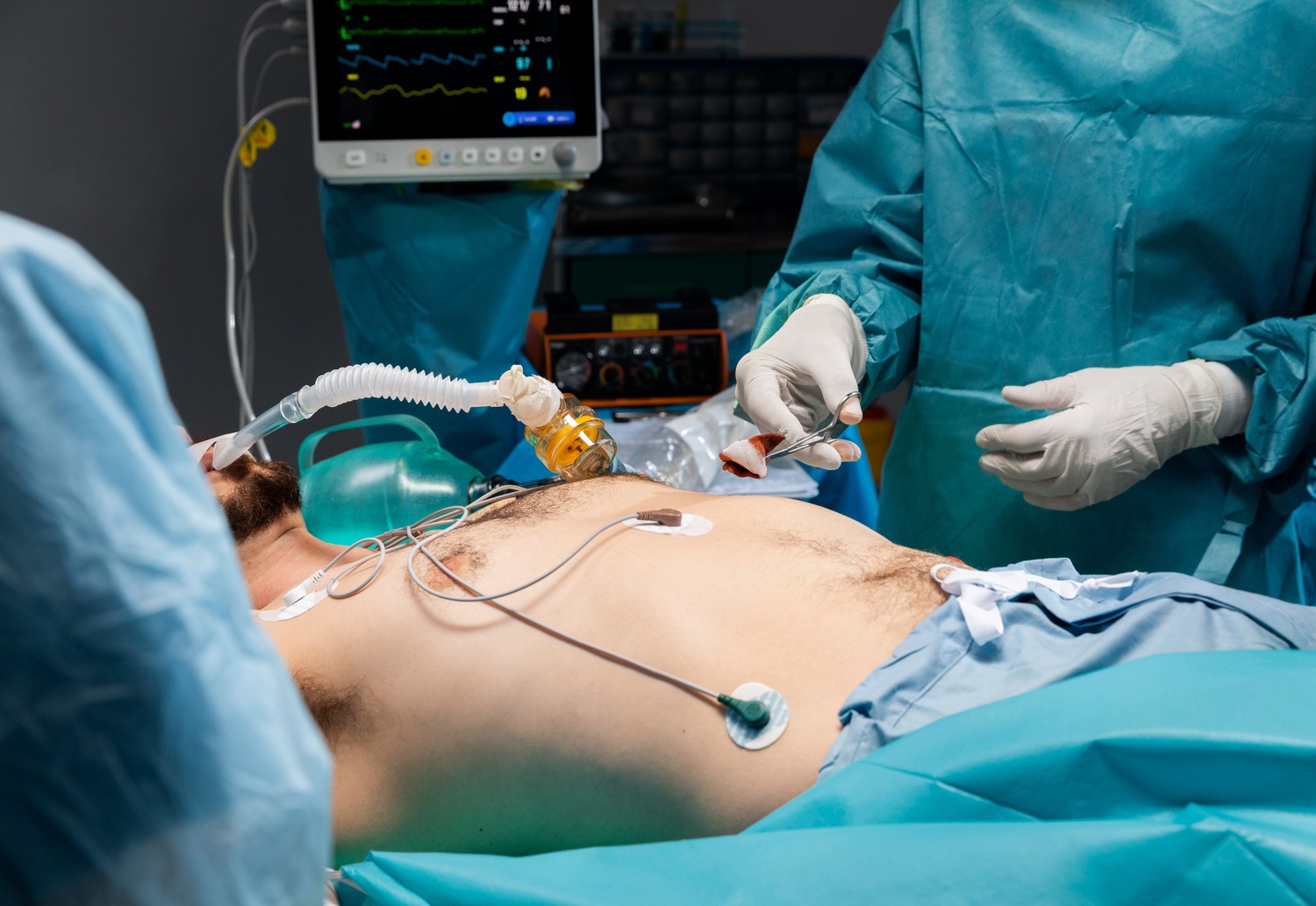
In an operating room, medical personnel perform meticulous surgery using highly specialised instruments to reduce endometrial lesions and attempt to enhance a woman's fertility performance.
Final Thoughts
Endometriosis is a persistent health issue for women and needs immediate management if recognised. Timely symptom identification of such conditions as pelvic pain, acute dysmenorrhea, and abnormal vaginal discharge can assist in early diagnosis and treatment. Effective therapies are now available through modern medical and surgical management, facilitating pain relief and fertility outcomes.
A comprehensive patient-centric treatment plan will help achieve a favourable prognosis and well-being in the long term. Adequate knowledge and early diagnosis contribute to better women's health outcomes.
Expert Care with Dr Shachi Singh
If you notice any of these symptoms related to Endometriosis and need help to diagnose or treat the condition effectively, please do not hesitate to consult an expert. Dr. Shachi Singh is an eminent Obstetrician, Gynecologist, and Laparoscopic Surgeon offering tailored management techniques and solutions including latest medical or surgical treatment modalities so that patients will be more comfortable, pain-free and will have the chance of having a child.
Book your consultation today.
Frequently Asked Questions(FAQs)
1. What does severe endometriosis look like?
Severe endometriosis (stage III-IV) involves widespread, deeply infiltrating implants, large ovarian cysts (endometriomas), dense adhesions and distortion of pelvic anatomy. Organs, most commonly ovaries, fallopian tubes, bowel and uterus, are adherent and often form a "stuck-on" appearance with associated inflammation and fibrosis, infertility, decreased organ mobility and function.
2. Which organs does endometriosis affect?
Endometriosis may severely damage organs, though it does not 'kill' organs. Organs most commonly affected are the ovaries, fallopian tubes, uterus, bowel and bladder, and pelvic peritoneum. Severe cases can cause decreased organ mobility and function through adhesions, inflammation and scarring; prolonged untreated cases could potentially impair fertility, result in bowel obstruction and/or urinary dysfunction and/or chronic pelvic dysfunction.
3. How painful is endometriosis pain?
Pain in Endometriosis varies significantly and can be severe and incapacitating. It may manifest as chronic pelvic pain, debilitating dysmenorrhea, painful intercourse and dyschezia/dysuria. This may or may not correlate with the stage of endometriosis; severity does not necessarily reflect extent, and its impact on the woman's quality of life may be very considerable.
4. What are the signs of severe endometriosis?
The signs are severe, chronic pelvic pain, heavy or irregular menses, deep dyspareunia, infertility, painful bowel function (dyschezia) and painful urinary function (dysuria), fatigue and gastrointestinal problems, and in the case of severe disease, ovarian cysts (endometriomas), adhesions and resultant organ dysfunction. Symptoms in more advanced disease may be persistent beyond menstrual cycles, worsening over time.
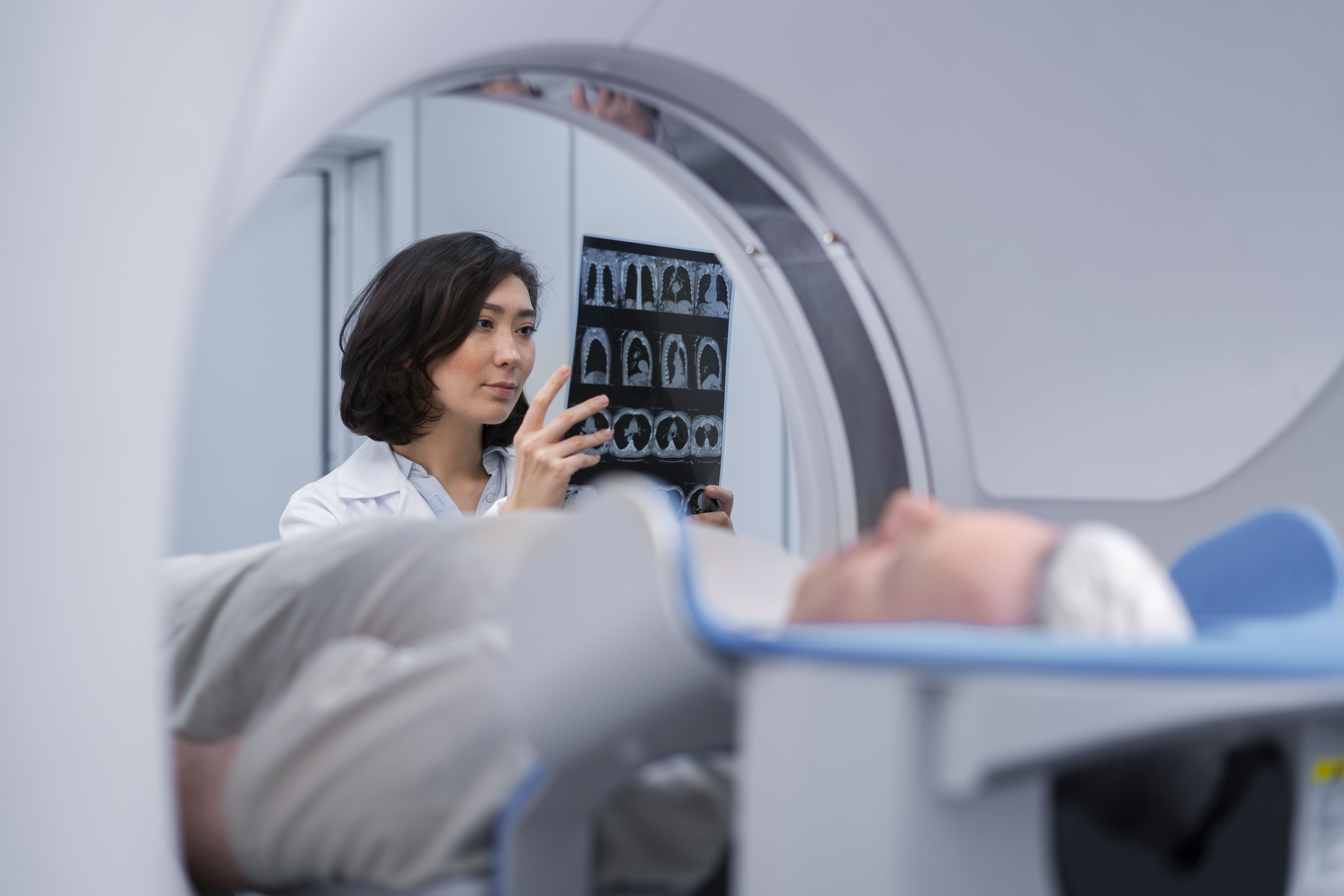
5. How do you tell if a woman has endometriosis?
The symptoms suggest a diagnosis of endometriosis in a female: chronic pelvic pain, dysmenorrhea, dyspareunia and infertility are the main indicators of potential endometriosis, though a gynecologist will make a suspected diagnosis on presentation with these symptoms. An ultrasound or MRI may aid the diagnosis with suggestive findings. A laparoscopic diagnosis and histological confirmation are required for an established diagnosis. Early presentation to the gynecologist is key to a positive diagnosis.