Cervical Cancer Prevention: HPV Vaccine and Screening

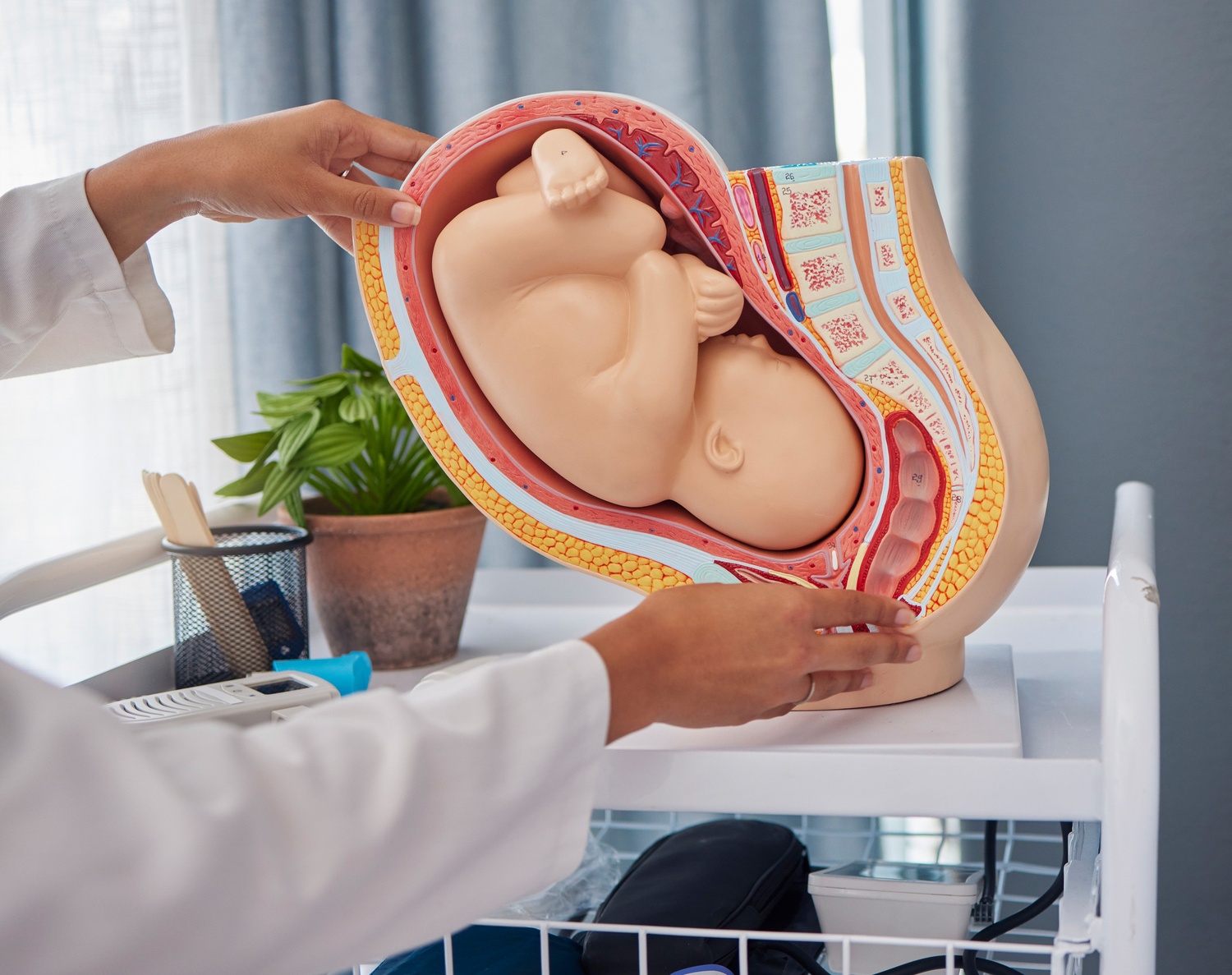
A diagram showing the process of Cervical Cancer development in the cervix and uterus following HPV infection.
Cervical cancer is the most preventable cancer in the world; however, it is one of the most problematic conditions for women worldwide. Most cases of cervical cancer are caused by long-term HPV infection. It is very fortunate, as HPV vaccination and screening programs have drastically decreased the prevalence of cervical cancer.
Cervical screening tests like the Pap smear are also useful for identifying pre-cancerous conditions before they grow. Increased knowledge of getting the correct vaccine and participating in cervical screening programs can be beneficial to improve the health of women globally and alleviate the effects of cervical cancer by promoting prevention.
What Is Cervical Cancer?
Cervical cancer is a malignancy of the epithelium of the cervix, where the squamous and columnar epithelia meet at the transformation zone, being the most frequent site of the neoplasia. Cervical cancer is the result of persistent infection by high-risk types of Human Papillomavirus, most frequently HPV 16 or HPV 18.
It is generally a slow process starting from the development of precancerous changes in cervical intraepithelial neoplasia, which, if left untreated, can develop into invasive cervical carcinoma. In terms of histology, it is most frequently classified as squamous cell carcinoma and as adenocarcinoma.
Early cervical cancer is often asymptomatic, while more advanced stages can cause abnormal bleeding, pelvic pain, and discharge, and so the crucial factor in terms of early diagnosis of this neoplasia is the screening programs and regular tests.
Causes And Symptoms Of Cervical Cancer
1. Cervical Cancer Causes
- Chronic infection with high-risk types of Human Papillomavirus, especially HPV-16 and 18.
- Early onset of sexual activity and numerous sexual partners increase the chance of contracting HPV.
- An impaired immune system (e.g. With HIV) makes it more likely that the virus will not be cleared by the body.
- Long-term use of Oral Contraceptive Pills is considered a possible small increase in risk for some women.
- Smoking causes damage to cells in the cervical epithelium.
- Poor genital hygiene and failure to attend for regular screening will mean that precancerous cell changes will not be picked up in their early stages.
2. Cervical Cancer Symptoms
- Abnormal vaginal bleeding (e.g. Bleeding after intercourse, between periods, or post-menopausal bleeding).
- Continuous offensive vaginal discharge caused by infection of the necrosis of the tumor.
- Pelvic pain or lower abdominal pain in more advanced stages.
- Dyspareunia (painful sexual intercourse).
- Unexplained weight loss, fatigue, and debility in later stages.
In early stages, there are often no symptoms at all, which reiterates the need for cervical screening.
Human Papillomavirus Infection (HPV) and Cervical Cancer

A graphic depicting several distinct microscopic viral patterns of the HPV virus structures.
Cervical cancer is strongly related to continuous Human papillomavirus infection; thus, preventative actions can be extremely effective. The invention of the HPV vaccine has led to a new age in preventative health, helping decrease the rate of cervical and other HPV-associated cancers, and working in conjunction with early screening for optimum prevention.
It is important to understand the advantages of vaccination, its requirements, and the need for continued screening to maintain reproductive health in the long term.
- HPV is responsible for the majority of cervical cancers. High-risk strains are typically HPV-16 and HPV-18.
- The vaccine is effective against strains of HPV that cause cancer and decreases the risk for vaginal, cervical, and vulvar cancers.
- Recommended for both preteen boys and girls ages 11-12; can be given to individuals as young as 9 years.
- Vaccination is recommended for all individuals up to age 26 who are not already vaccinated.
- Vaccination for adults aged 27-45 may be given following a discussion with the provider about the individual's specific needs.
- A two-dose vaccination schedule is recommended before age 15. Three doses are necessary for those vaccinated 15 years of age and older.
- The vaccine does not treat any current HPV infections, warts, or cancer. It protects against new HPV infections.
- Women are still required to have regular screenings after being vaccinated for the early detection of cervical cancer.
Therefore, both vaccination and cervical screening significantly decrease the risk of contracting cervical cancer and other health-related concerns due to this disease.
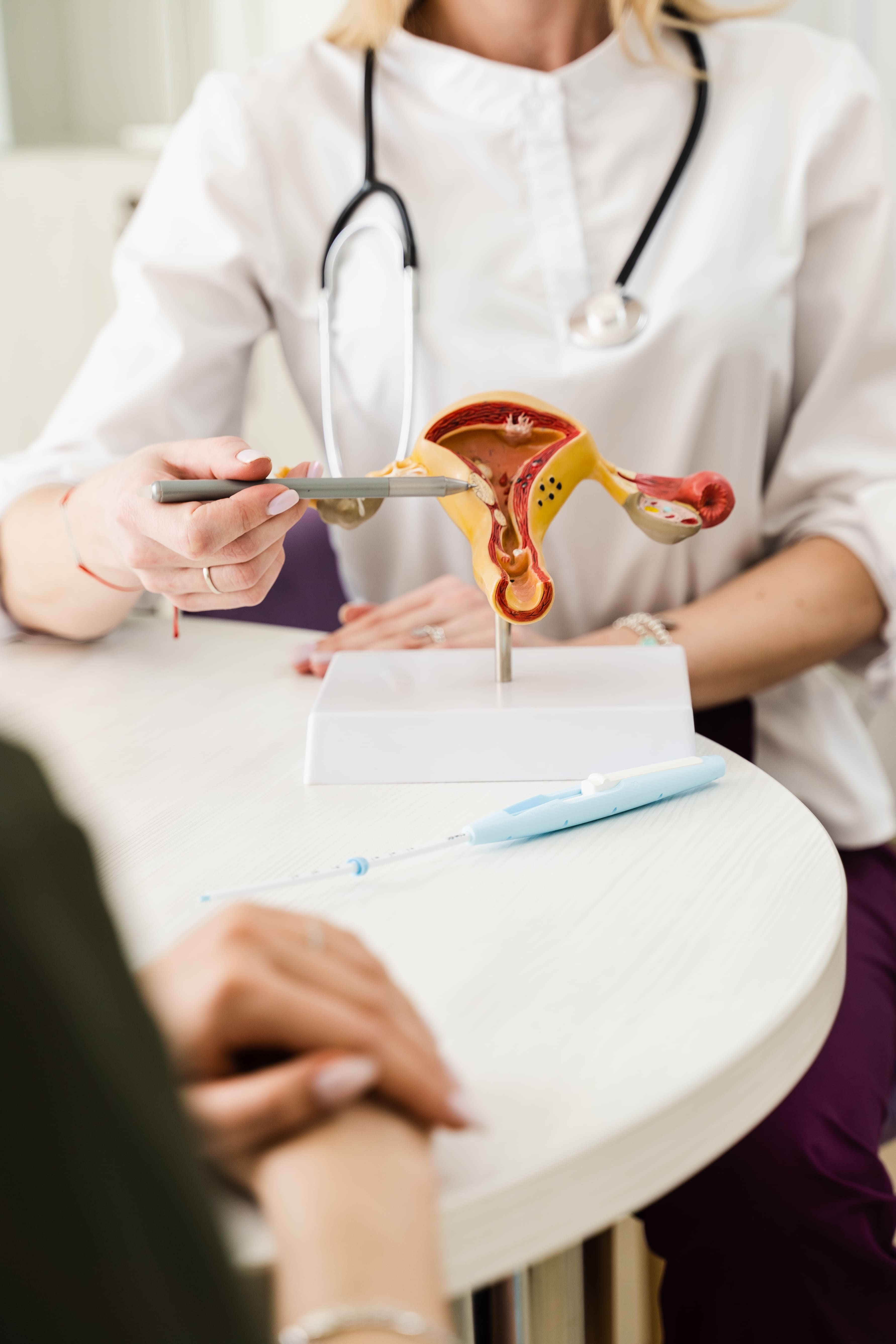
Cervical Cancer Screening Tests
- Pap Test (Pap Smear) - A sample of cells is collected from the surface of the cervix during a pelvic exam using a small, soft brush or spatula. Under the microscope, the cells are analysed for abnormality (e.g., dysplasia or precancerous condition). The test takes just a few minutes and should not be uncomfortable. Routine Pap smears can detect early changes in the cells of the cervix before they become cancerous.
- HPV Test - This test determines if a high-risk strain of the human papillomavirus (HPV) is present in the cervical cells. Cells are gathered, similar to a pap smear, and then tested using molecular techniques in a lab. The test helps to detect women at increased risk before cellular abnormalities appear.
Prevention of Cervical Cancer
- Age-appropriate HPV vaccination is encouraged to prevent acquisition of oncogenic HPV types.
- Regular cervical screening with the combination Pap and HPV testing should be practiced to identify and treat precancerous lesions.
- Safe sexual practices, including regular condom use, are important for the prevention of HPV acquisition.
- Fewer sexual partners, and hence reduced exposure, is important.
- Smoking increases local immune suppression and cervical cell damage, and should be avoided.
- Proper genital hygiene and general health are necessary.
- Early diagnosis and treatment of any cervical lesions or infection must be ensured.
Final Thoughts

A health-themed layout featuring a stethoscope, a clipboard, a paper cutout of a uterus, and a small flower on a blue background.
The combination of timely vaccination, screening, and awareness about its causes can eliminate cervical cancer. A continuous HPV infection leads to cancer, but screening (Pap and HPV tests) identifies pre-cancerous stages early. Certain things to avoid, like smoking, along with practicing safe sex and going for regular checkups, lower your risk significantly.
When all women have access to correct information, there will be a definite dip in cervical cancer. The combination of prevention and screening offers hope to fight this dreadful cancer, so that we can make it a thing of the past.
Expert Care With Dr. Sachi Singh
Thinking you might be due for cervical screening, or contemplating HPV vaccination? It's always the best time to speak with a doctor and a highly experienced Gynaecologist in Noida, Dr. Shachi Singh, who also excels as a Laparoscopic Surgeon, can offer well-informed medical advice for effective treatment.
Her patients have trusted her for more than 15 years of expertise in gynecology and obstetrics for precise diagnosis and sympathetic care, both in Noida and in the wider Delhi NCR region. Schedule your appointment today and take a proactive approach to women's health.
Frequently Asked Questions
1. Can cervical cancer be completely prevented?
Cervical cancer can be prevented to a large degree with vaccination against HPV and regular cervical cancer screening (Pap tests and HPV tests).
2. At what age should cervical cancer screening begin?
Cervical cancer screening generally begins at the age of 21 and continues regularly as determined by your doctor.
3. Is the HPV vaccine useful in adults?
The HPV vaccine can still provide benefits to adults up to age 45, depending on the specific patient and the physician's recommendation.
4. Do I need regular Pap tests even after getting vaccinated for HPV?
Regular Pap tests are still recommended, as vaccination does not protect against the occurrence of early cell changes.