Vaginal Atrophy: Causes, Symptoms, and Treatments

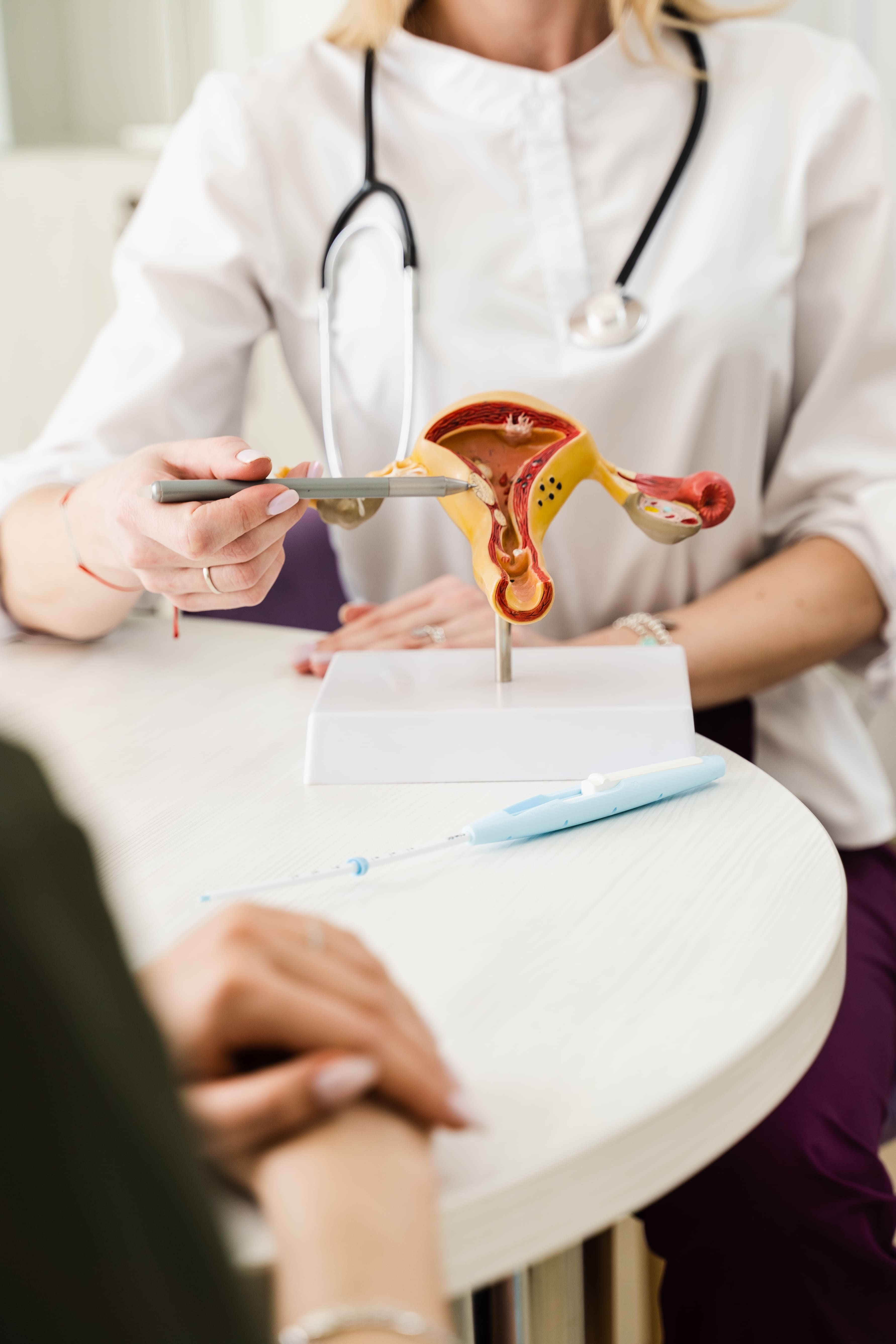
A gynaecologist uses a model of a woman's uterus to explain what happens to vaginal tissue and the changes in menopause.
Genitourinary Syndrome of Menopause (GSM), also called vaginal atrophy, is a frequently seen, but still largely unnoticed, condition among women, especially menopausal women. The condition results from a decrease in estrogen level, which results in vaginal wall atrophy, dryness and inelasticity of the vaginal tissues.
These physical alterations lead to vaginal discomfort, irritation and pain during routine daily life or sex. Besides vaginal problems, Urinary symptoms can also occur, causing diminished quality of life. With better education and appropriate intervention timelymannern, vaginal atrophy is treatable and can make women regain their comfort, confidence, and sex life.
What Is Vaginal Atrophy?
Vaginal atrophy is often more commonly known today as genitourinary syndrome of menopause or GSM. Vaginal atrophy occurs when lower levels of estrogen affect the vaginal lining; this causes vaginal tissue to thin out, dry, and become less elastic.
Lower estrogen levels typically happen during perimenopause and menopause, but they can also be caused by medical therapies or surgery to remove the ovaries. A reduction in estrogen does affect the vaginal tissues but also affects the urinary tract, and can cause a range of physical discomforts which effect day-to-day life.
- It commonly affects women approaching perimenopause and menopause
- Women with this disease suffer from dryness of the vagina, irritation and thinning of the vaginal walls
- Intimate acts will be affected, as the individual may suffer pain during intercourse (dyspareunia)
- Symptoms also often include those which are related to the urinary tract, such as urinary infection and incontinence
- It is considered that nearly 50% of women who reach menopause will experience the condition
- The problem affects day-to-day life and intimate relationships
Vaginal atrophy is an extremely common menopausal complaint as a result of the reduction in estrogen. It impacts both the urinary system and vaginal health and can cause irritation, discomfort and dryness in the vagina. Treatment initiated early can be effective in reducing the symptoms.
Causes Of Vaginal Atrophy (GSM)
1. Lowering Estrogen Levels In Menopause
A natural decline in estrogen levels at menopause is the primary reason for Vaginal Atrophy or GSM. It is estrogen that keeps vaginal tissues thick, moist, and elastic; a drop can make vaginal tissues thin, dry and inflexible, causing pain.
2. Altered Vaginal Flora Environment
With lower levels of estrogen, women can suffer from the lack of vaginal moisture (secretion) and from the imbalance of the vagina's normal acidic PH. This increases the delicacy of the vaginal tissues, rendering them more easily irritated and susceptible to infections.
3. Surgical & Treatment-Induced Causes
Certain medical treatments, like radiation therapy or chemotherapy, can affect the level of hormones produced by your body. Surgery of the ovaries would remove all hormonal stimuli.
4. Other Hormonal Fluctuations
The hormonal decline can also occur in breastfeeding women, leading to temporary vaginal dryness.
Symptoms of Vaginal Atrophy (GSM)
1. Changes In The Vagina
The most common change in the vagina caused by atrophy is dryness due to diminished lubrication, most frequently discovered during intercourse.
Thinning and irritation to the lining of the vagina cause an internal sensation of burning and discomfort. Frequent, ongoing itching in the vaginal cavity is a common complaint.
2. Painful Or Itchy Sex
Dyspareunia, pain during intercourse, is common as the elasticity of the vaginal walls decreases and dryness sets in. Spotting or bleeding after sex can also be experienced by some women.
3. Abnormal Discharge And External Itchings
Changes in vaginal discharge are possible, often developing into a yellowish discharge. An external irritation and itching in the vulvar region of the vagina may also arise.
4. Urinary Symptoms
In some cases, vaginal atrophy causes effects in the urinary tract, leading to recurrent UTIs. A frequent urge to urinate, or increased frequency of urination, may occur. Urinary incontinence, burning when urinating (dysuria), pain when passing urine, or blood in the urine (hematuria) can all develop due to vaginal atrophy.

A woman in discomfort from urinary problems standing beside a toilet, showing symptoms from vaginal atrophy.
Treatment And Management Of Vaginal Atrophy
1. Hormonal Therapies
- Hormonal therapy is generally the most effective way to treat vaginal atrophy. It can be administered either locally or systemically.
- Topical and local administration of hormones includes the use of vaginal creams, vaginal tablets, or vaginal rings, which deliver a low dose of estrogen directly to the tissues of the vagina to improve moisture, tissue thickness and elasticity without significantly impacting the levels of estrogen throughout the body.
- Systemic hormonal replacement therapy (HRT) may be prescribed for those women with multiple menopausal symptoms, including night sweats and other symptoms such as mood swings and sleep problems.
2. Non-Hormonal Treatments
- There are non-hormonal methods available to women who cannot, or are unwilling, to receive hormonal therapy.
- Vaginal lubricants are commonly used to aid with intercourse and decrease discomfort. Vaginal moisturisers are another alternative to aid in improving lubrication.
- Some natural oils can be used, including olive or coconut oil,l to help ease vaginal dryness.
3. Additional Therapies
- Vaginal dilators may be used to help stretch the vagina so it may become more elastic.
- Oral ospemifene is one drug which has the effect of acting like oestrogen in the tissues of the vagina, without the oestrogen actually present.
4. Long-Term Care And Prognosis
- Regular consultation with a doctor is vital in tracking progress and altering treatment.
- The use of multiple approaches often helps alleviate symptoms to a considerable degree.
When To Seek A Doctor’s Help?
- Continuous vaginal dryness, burning or itching that doesn't resolve with simple home treatment
- Pain during intercourse (dyspareunia) is preventing you from enjoying sex and causing discomfort.
- Unusual vaginal discharge with a yellowish hue or foul odour
- Spotting or bleeding after sexual intercourse, or between menstrual cycles
- Frequent UTIs or constant need to urinate
- Burning or pain during urination (dysuria)
- Inability to control urination (urinary incontinence)
- Blood in urine (hematuria)
- Symptoms that are negatively impacting your daily activities, sleep and emotional state
- Over-the-counter lubricants and vaginal moisturisers are not effective.
Final Thoughts
Vaginal atrophy does not have to be a problem that every woman is willing to live with; it is treatable, and it should not just be part of natural ageing. The condition is most common around menopause and is likely to affect a woman's body, state of mind, and sex life quite dramatically.
Early diagnosis and treatment with appropriate therapy (hormonal or non-hormonal) are most likely to bring relief. Discussion with the health professional is important to gain an effective and individual treatment plan. The majority of women may see major changes to the symptoms, and women would be healthy, active, comfortable and free from limitations with the correct treatment.
Expert Care With Dr Shachi Singh
If you are suffering from any of the symptoms of vaginal atrophy, getting prompt medical attention from a skilled physician could go a long way in managing your condition and alleviating your concerns. Dr Shachi Singh, senior consultant gynaecologist in Noida, is a highly experienced professional with more than 15 years in women's healthcare.
She specialises in complex surgical techniques such as laparoscopy and minimally invasive surgery, hysteroscopy, handling high-risk pregnancies, performing fertility procedures and also cosmetic gynaecology. She is renowned among patients for her dedicated and patient-friendly approach and provides advanced, effective and highly individualised solutions for better sexual wellness as well as overall health of women. So, book your consultation today.
Frequently Asked Questions (FAQs)
1. Does vaginal atrophy hurt?
Yes, due to the lack of estrogen, the vaginal tissues may become thin, dry and inflamed, causing soreness, discomfort and burning, which is usually aggravated by activity such as walking or sitting, and exacerbated by urination and intercourse.
2. How much does vaginal atrophy pain hurt?
The level of pain ranges from slight irritation to considerable discomfort. Many women develop dyspareunia (painful intercourse) and a burning or tender sensation. If untreated, the condition will not reverse itself, and the symptoms will worsen, interfering with daily life and intimacy.
3. Can vaginal atrophy be reversed?
Vaginal atrophy cannot always be reversed, but it can be successfully treated. Topical estrogen treatments (applied vaginally), moisturisers, and lubricants can replenish natural moisture levels, restore healthy tissue and minimise the discomfort as well as any associated urinary problems.
4. How can I tell if I have vaginal atrophy?
The common symptoms include dry, itchy or burning vagina and pain during intercourse. There is often reduced vaginal lubrication. Other signs of vaginal atrophy can include frequent infections, burning upon urination, increased urge to urinate, and pain upon urination. The symptoms will be confirmed by a doctor or healthcare professional after examination.